Appendicitis misdiagnosis is a surprisingly common and devastating event. When emergency doctors fail to identify this surgical emergency, patients face risks like a ruptured appendix, sepsis, and even death.
Key Facts About Appendicitis Misdiagnosis:
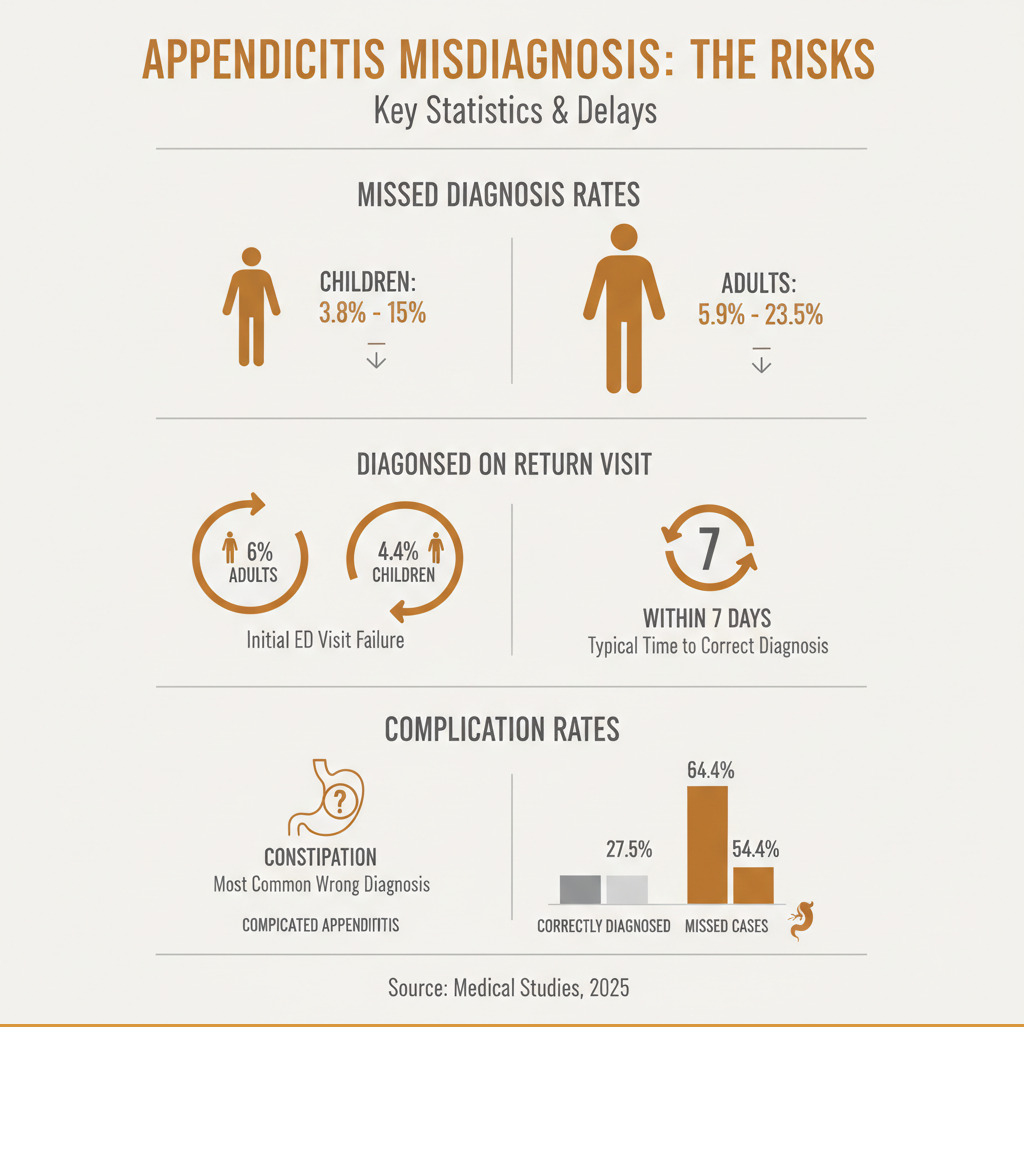
- Children: Missed in 3.8% to 15% of ED visits
- Adults: Missed in 5.9% to 23.5% of ED visits
- Initial Visit Failure: 6% of adults and 4.4% of children are misdiagnosed on their first visit
- Most Common Misdiagnosis: Constipation
- Serious Complications: 54.4% of missed cases develop complicated appendicitis vs. 27.5% in correctly diagnosed cases
Appendicitis is one of the most frequent urgent surgical emergencies, yet emergency departments continue to send patients home with the wrong diagnosis. Behind each statistic is a real person—a parent told they have “gastroenteritis” or a child dismissed with “constipation” while their appendix is nearing rupture.
Many of these errors are preventable. Studies show that relying on abdominal X-rays instead of more accurate CT scans increases the risk of a missed diagnosis. Communication breakdowns between emergency physicians and radiologists also contribute to these dangerous oversights.
For families dealing with the aftermath, the toll is overwhelming. A missed diagnosis often leads to longer hospital stays, more surgeries, permanent complications, and staggering medical bills. What should be a routine procedure can become a fight for survival.
The Scope of Appendicitis Misdiagnosis
Appendicitis misdiagnosis happens far more often than expected for such a common condition. Between 3.8% and 15% of children and 5.9% to 23.5% of adults leave the emergency department with an incorrect diagnosis. For an adult with appendicitis, this means there’s nearly a one-in-four chance of being sent home with the wrong answer.
Many of these patients must return to the hospital to get the right diagnosis. About 6% of adults and 4.4% of children are not diagnosed correctly until a second visit, usually within seven days of being misdiagnosed. When an appendix is inflamed, every hour counts, making this delay dangerous. If the appendix becomes too infected, it can rupture or burst, causing the built-up infection to spill into the abdominal cavity. When this happens, massive internal infection including septic shock can occur within hours and it immediately becomes a life-threatening emergency. For a deeper look at the factors behind these errors, scientific research on factors associated with missed diagnosis offers valuable insights.
How Often is Appendicitis Misdiagnosed?
The most common incorrect diagnosis is constipation. Patients are told they are backed up when the problem is far more serious. This delay is critical: patients misdiagnosed on their first visit wait a median of 29.5 hours for surgery, compared to just 9.3 hours for those diagnosed correctly. That extra 20 hours significantly increases the risk of rupture.
Who is Most at Risk for a Missed Diagnosis?
Certain groups face a higher risk of appendicitis misdiagnosis.
- Age: Patients with a missed diagnosis tend to be older (median age of 29 vs. 23), as they often don’t present with “textbook” symptoms.
- Gender: Women who are misdiagnosed are often admitted to a non-surgical department because their symptoms can mimic gynecological issues. Men are more likely to be sent home entirely.
- Pre-existing Conditions: The risk skyrockets for patients with other health problems. The missed diagnosis rate for adults with multiple comorbidities is 58.0% compared to 30.5% for healthier patients. For children, it’s 12.4% versus 5.0%. A complex medical history can distract doctors from considering appendicitis.
If you are older, female, or have other health issues, it is vital to be persistent about your abdominal pain and advocate for a thorough evaluation.
Why Appendicitis is So Often Misdiagnosed
Why do doctors miss such a common diagnosis? The reality is that appendicitis misdiagnosis often results from a combination of medical complexity and patients who don’t fit the textbook description.
Appendicitis doesn’t always present clearly. The “classic” symptoms—pain moving from the belly button to the lower right side, with nausea and fever—are often absent. Many patients arrive with vague symptoms that could indicate dozens of other conditions, from a stomach bug to a UTI. This puts emergency physicians in a tough spot, trying to differentiate appendicitis from a long list of possibilities.
Cognitive biases can also lead to errors. Premature closure occurs when a doctor settles on a diagnosis too quickly, like “constipation,” and stops considering other options. Anchoring bias is similar, where a first impression becomes difficult to shake, causing the doctor to unconsciously ignore contradictory symptoms. These mental shortcuts are common in high-pressure environments but can be dangerous when diagnosing appendicitis.
Challenges in Diagnosing Specific Populations
Some groups are at higher risk because their symptoms are atypical.
- Children: Young children can’t always describe their pain clearly, often just saying their “tummy hurts.” This communication barrier makes it easy to mistake appendicitis for a simple stomach bug.
- Elderly Patients: Older adults may have a blunted pain response and vague symptoms that are attributed to other health issues. Delays in this group are especially dangerous, with mortality rates from appendicitis climbing as high as 5% to 15%.
- Pregnant Women: As the uterus grows, it pushes the appendix, changing the location of the pain. Normal pregnancy symptoms like nausea and abdominal discomfort overlap with appendicitis, making diagnosis extremely challenging. For more on this, read about appendicitis in pregnancy from the National Library of Medicine.
The Impact of Atypical Symptoms on Appendicitis Misdiagnosis
When patients don’t follow the script, the risk of misdiagnosis rises. Many who are misdiagnosed report pain in the upper abdomen or have no fever or nausea. When hallmark symptoms are missing, doctors consider more common explanations.
- Gastroenteritis (stomach flu) is a frequent misdiagnosis, as both can cause abdominal pain, nausea, and vomiting.
- Urinary tract infections (UTIs) can mimic appendicitis, especially in women, with lower abdominal pain.
- Constipation remains one of the most common incorrect diagnoses for abdominal pain and bloating.
When symptoms are atypical, treatment is delayed. With appendicitis, this delay increases the chance of rupture, abscess, and sepsis, turning a routine issue into a life-threatening emergency.
The Role of Diagnostics and Systemic Failures
When you go to an ED with severe abdominal pain, you trust the hospital has the right tools and systems. However, appendicitis misdiagnosis often stems from which tests are ordered and how the results are communicated.
How Diagnostic Imaging Affects Appendicitis Misdiagnosis
Not all imaging is equal. Research shows patients who only received abdominal X-rays were far more likely to have their appendicitis missed. X-rays simply lack the detail to reliably identify an inflamed appendix.
CT scans, however, are highly accurate. Before their widespread use, about one in four appendectomies were unnecessary. Now, that rate is just 1-3%. But even the best technology fails if results aren’t interpreted or communicated properly. A vague report from a radiologist or a breakdown in communication with the ED physician can lead to a missed diagnosis. Effective closed-loop communication—where critical findings are confirmed as received and understood—is essential to prevent these errors.
System-Level Improvements to Reduce Diagnostic Errors
Preventing errors requires systemic change, as diagnostic mistakes affect an estimated 12 million Americans annually. Key improvements include:
- Standardized Diagnostic Protocols: These give physicians a clear, evidence-based roadmap for evaluating patients with suspected appendicitis, ensuring consistent care.
- Clinical Decision Support Tools: Scoring systems like the Alvarado score and the Pediatric Appendicitis Score help doctors assess risk more objectively by combining symptoms, lab results, and exam findings.
- Clear Follow-Up and Discharge Instructions: What happens after you leave the ED is critical. Patients need specific instructions on which symptoms warrant an immediate return, rather than vague advice to “come back if it gets worse.” This creates a safety net for uncertain cases.
- Continuous Education: Regular training on diagnostic pitfalls, atypical presentations, and cognitive biases helps keep providers vigilant.
When hospitals implement these improvements together, they create multiple layers of protection against appendicitis misdiagnosis. At Garmey Law, we see the human cost when these systems fail—unnecessary suffering and devastating complications from preventable harm.
Consequences and Legal Implications of a Missed Diagnosis
A delayed diagnosis of appendicitis is a medical emergency that worsens by the hour. When an inflamed appendix bursts (ruptured appendix), infection spreads throughout the abdomen, changing a manageable situation into a life-threatening crisis.
This can lead to dangerous complications like perforation (a hole in the appendix), abscess formation (pockets of infection), and sepsis (a body-wide inflammatory response that can cause organ failure or death). These issues mean longer hospital stays, more invasive surgeries, and overwhelming medical bills.
The Severe Health Risks of a Delayed Diagnosis
The data is clear: 54.4% of patients with missed appendicitis develop complicated appendicitis, compared to just 27.5% of those diagnosed correctly on the first visit. These patients endure increased pain and face long-term complications like chronic pain or bowel obstructions from internal scarring. In the most tragic cases, a missed diagnosis can lead to wrongful death.
Medicolegal Landscape of Appendicitis Malpractice
Appendicitis misdiagnosis is a leading cause of emergency department malpractice lawsuits, accounting for about 10% of all closed claims. In radiology, it’s the third most commonly missed GI diagnosis, with over 60% of these cases resulting in payments to injured patients.
| Outcome Measure | Timely Diagnosis (Median) | Missed Diagnosis (Median) |
|---|---|---|
| Time to Surgery | 9.3 hours | 29.5 hours |
| Complicated Appendicitis | 27.5% | 54.4% |
Table based on data from Ochsner Journal 2023 study
This table highlights the danger of delay: patients wait over three times longer for surgery, and the complication rate nearly doubles.
To win a malpractice claim, you must prove four elements: a duty of care existed (doctor-patient relationship), the provider breached the standard of care (negligence), this breach caused your injuries, and you suffered actual damages (medical bills, lost wages, pain and suffering). For more on legal precedents, you can review legal precedents in appendicitis malpractice.
If you’ve been harmed by a missed appendicitis diagnosis, you deserve answers. Garmey Law has experience in medical malpractice representation and fights to get clients the compensation they need. You shouldn’t have to steer the complex legal process alone.
Frequently Asked Questions about Appendicitis Misdiagnosis
Dealing with abdominal pain and a potential appendicitis misdiagnosis can be frightening. Here are answers to common questions.
What are the classic symptoms of appendicitis?
Classic signs often include:
- Pain that starts near the navel and moves to the lower right abdomen.
- Nausea and vomiting.
- Loss of appetite.
- A low-grade fever.
- Tenderness in the lower right abdomen.
However, many people have atypical symptoms, which contributes to appendicitis misdiagnosis.
What should I do if I’m sent home from the ED but my abdominal pain worsens?
If your symptoms worsen after being sent home, seek immediate medical attention.
- Return to the emergency department without delay.
- Clearly explain your history: State that you were seen before and describe how your symptoms have changed or intensified.
- Advocate for more testing: Politely but firmly request further evaluation, like a CT scan, if you feel your concerns are being dismissed.
Trust your instincts. Persistent or worsening pain is a serious warning sign.
Can I sue a hospital for misdiagnosing appendicitis?
Yes, you may have grounds for a medical malpractice lawsuit if the appendicitis misdiagnosis was due to negligence and caused you harm. A successful claim must prove:
- Breach of the standard of care: The provider failed to act as a reasonably competent professional would have.
- Causation and harm: The negligence directly caused your injury, such as a ruptured appendix, leading to additional surgeries, prolonged illness, or wrongful death.
These cases are complex and have strict deadlines (statutes of limitations). If you believe you were harmed by an appendicitis misdiagnosis in Maine, consulting an experienced medical malpractice attorney is a critical first step.
Protecting Yourself From Appendicitis Misdiagnosis
When you seek emergency care for severe abdominal pain, you place your trust in the medical system. Yet, appendicitis misdiagnosis happens far too often, with devastating consequences. As this article has shown, a significant percentage of both children and adults are sent home incorrectly diagnosed, only to return later in critical condition. What should be a routine surgery can escalate into a fight for life against sepsis, abscesses, and other complications.
Preventing these errors requires systemic change: standardized diagnostic protocols, clear communication between medical teams, and proper use of imaging like CT scans. Doctors must also remain vigilant against cognitive biases that can lead to mistakes.
While the healthcare system works to improve, patient advocacy is crucial. If you are sent home but your pain worsens, return to the ED immediately. Speak up about your symptoms and request further testing if you feel something is wrong. No one knows your body better than you do.
At Garmey Law, we have seen how appendicitis misdiagnosis shatters lives. We represent the “underdogs”—patients and families facing off against large hospital systems after a preventable medical error. We bring aggressive advocacy and genuine compassion to every case, fighting to hold negligent parties accountable.
If you or a loved one in Maine has suffered due to a delayed or missed appendicitis diagnosis, we want to hear your story. We will investigate your case thoroughly and fight to secure the compensation you deserve.
Contact a medical malpractice attorney at our firm today for a confidential consultation. You do not have to face the consequences of medical negligence alone.