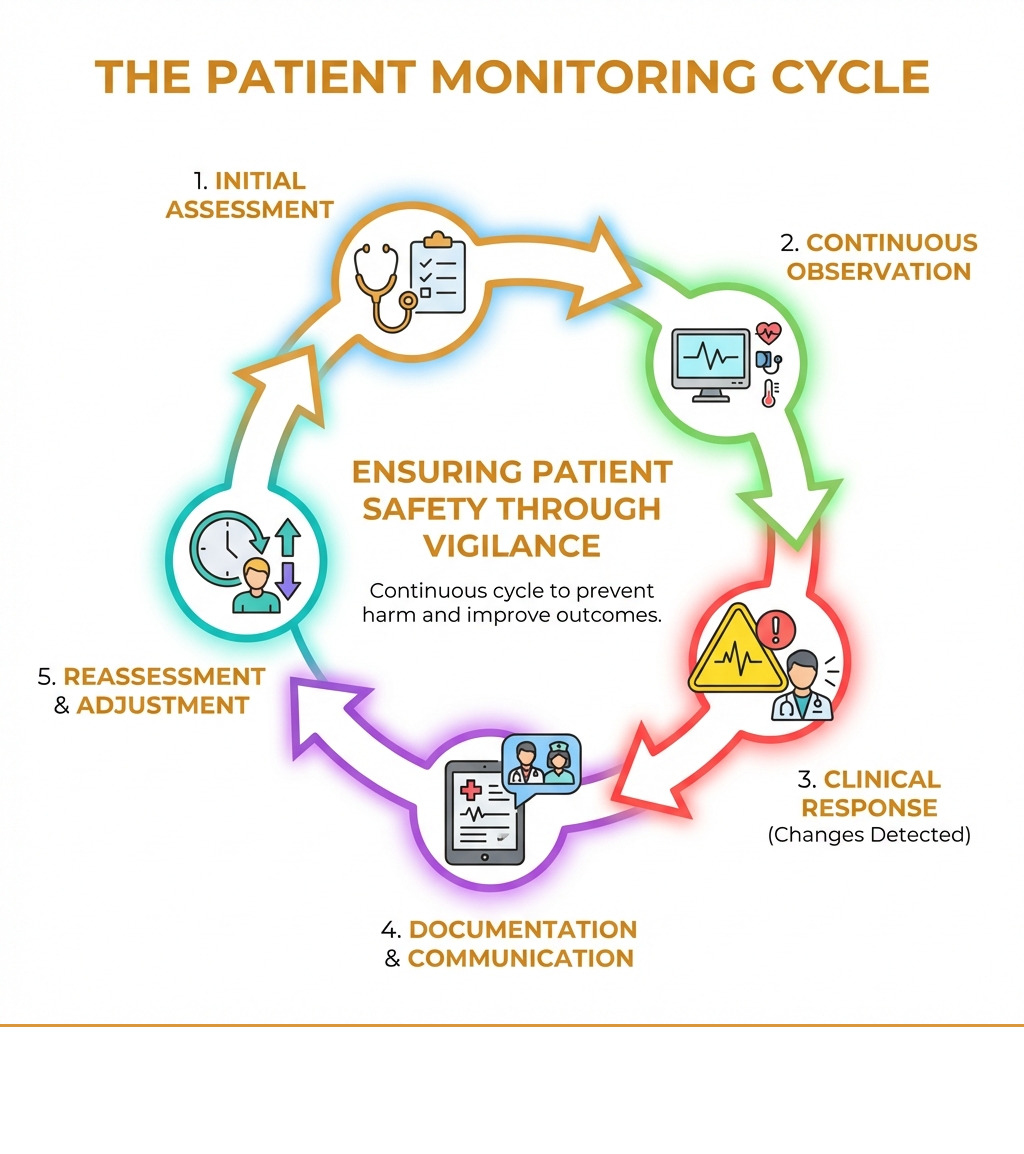
When a patient is under the care of a healthcare facility or nursing care facility, that patient is reliant on the healthcare provider to take certain precautions and make sure they are not exposed to hazards within the healthcare provider’s control. Failure to monitor occurs when healthcare providers neglect to observe and assess a patient’s condition consistently, missing critical changes in vital signs, ignoring symptoms, or failing to respond to medical device alarms. It also occurs when a patient who should have eyes on them at all times end up alone and suffer an injury from trying to do something that otherwise they should have received assistance doing, like going to the bathroom alone if they are a fall risk. This form of medical negligence can lead to preventable complications including sepsis, brain damage, cardiac arrest, traumatic injuries to organs or fractures to bones, and even death.
What Failure to Monitor Includes:
- Leaving patients unattended for extended periods without vital sign checks
- Ignoring electronic alerts or equipment alarms signaling dangerous changes
- Missing communication during shift handoffs between medical staff
- Failing to follow physician orders for monitoring frequency
- Not recognizing or responding to patient complaints or deteriorating conditions
- Neglecting to track critical measurements like blood sugar, oxygen levels, or fetal heart rate
When you trust a hospital or medical facility with your care, you expect nurses and doctors to watch for warning signs before they become emergencies. But when staffing shortages, ignored alarms, or communication breakdowns cause providers to overlook dangerous changes, patients suffer consequences that could have been prevented. Garmey Law has resolved tens of millions of dollars in cases for clients who have been inappropriately monitored or suffered injuries from lack of appropriate attention from medical providers, doctors, nurses, or hospital systems.
Peter Richard and Alexis Garmey Chardon, trial attorneys at Garmey Law with extensive experience representing victims injured by medical negligence, have seen how failure to monitor patients causes devastating, preventable injuries to patients and families across Maine. Their practices focuses on holding healthcare providers accountable when monitoring lapses lead to catastrophic harms.
Understanding Failure to Monitor in a Medical Context
When we talk about failure to monitor, we are talking about a breakdown in one of the most basic promises of healthcare: “We will watch over you.” In a medical context, monitoring is the continuous process of observing a patient’s physiological state to ensure they are stable and responding well to treatment. It is not optional – it is a legal and professional duty of care owed to every patient.
Defining the Duty to Monitor
Every healthcare provider, from the surgeon in the operating room to the nurse on the night shift in every hospital, urgent care, doctor’s office, nursing home, dementia unit, skilled nursing facility, or memory care unit has a duty to monitor the patients relying on their care. This duty is defined as the “standard of care” – what a reasonably competent healthcare professional would do in the same situation, or what no reasonably competent healthcare professional would omit doing in the same situation.
Monitoring is not passive. It requires clinical judgment, appropriate staffing, and systems designed to ensure that patients are not neglected. A nurse does not just look at a screen; they interpret what a dropping blood pressure reading means in the context of a patient who just came out of surgery. If a patient is high-risk, the provider may need to increase the frequency of checks based on changes in condition and facility protocols, and to escalate concerns when needed. Patient rounding schedules serve the purpose of ensuring that every patient receives consistent supervision and attention. When that does not occur, or even worse when it is documented it occurred but the medical records show that critical medical situations were missed during those rounding records, medical negligence may have occurred.
The Role of Medical Technology
Modern medicine relies heavily on technology. We have pulse oximeters to track oxygen, telemetry units for heart rhythms, and sophisticated alarms for IV pumps. However, technology is only as good as the humans responding to it.
Monitors and electronic alerts are designed to be a first line of defense. When a patient’s oxygen levels dip or their heart rate spikes, these machines beep and flash. Failure to monitor often involves “alarm fatigue,” where staff become desensitized to constant noise in a busy ward and begin to ignore or silence alerts without properly checking the patient. When technology is ignored, the safety net disappears.
Common Scenarios and Consequences of Negligence
The consequences of failing to watch a patient can be swift and permanent. When a condition is not caught early, a minor complication can spiral into a life-threatening emergency. In our work across Maine, York County to Aroostook County, we see several recurring scenarios where these lapses occur.
Failure to Monitor During Labor and Delivery
Childbirth is a time when constant vigilance matters for both mother and baby. Fetal heart rate monitoring is commonly used to help the care team identify signs that a baby may not be getting enough oxygen.
If a nurse or doctor fails to recognize non-reassuring fetal heart patterns – such as minimal variability or late decelerations – the baby may suffer oxygen deprivation. This can lead to Hypoxic-Ischemic Encephalopathy (HIE) or cerebral palsy. Proper monitoring can enable timely interventions, like an emergency C-section, that may prevent lifelong disability.
Failure to Monitor in Post-Operative and Inpatient Care
The hours following surgery are high-risk. Patients are often under the influence of anesthesia and pain medication, which can mask symptoms of internal bleeding or respiratory distress.
Common post-op monitoring failures include:
- Pulmonary Embolism (PE): Failing to monitor mobility or prevention measures can contribute to blood clots that travel to the lungs.
- Hypoglycemia: Failing to check blood sugar in diabetic patients can lead to loss of consciousness and irreversible brain injury.
- Sepsis: If temperature, heart rate, and other warning signs are not tracked and acted on, an infection can progress to septic shock.
Psychiatric and Long-Term Care Oversight
Monitoring is not only about vitals; it is also about safety. In psychiatric settings, providers must monitor patients for self-harm risks. In Maine, care facilities have faced scrutiny when residents with dementia or mental health struggles elope (wander away) because they were not being properly supervised. Psychiatric malpractice can involve a failure to maintain a safe environment or failing to check on a patient at the intervals required by their care plan.
Why Healthcare Providers Fail to Monitor Patients
It is rarely a case of a “bad” person intentionally ignoring a patient. Instead, failure to monitor is usually the result of systemic breakdowns within a hospital or nursing home. These failures often are the result of overworked staff and medical decisions made for the purpose of moving as many patients through a system as possible rather than focusing on providing excellent individualized care to the patients in front of the providers or nurses.
Systemic Failures in Maine Facilities
Many facilities in Maine, including those in Maine’s largest cities like Portland, Lewiston and Auburn, Bangor, and Augusta, struggle with staffing ratios. When one nurse is responsible for too many patients, the quality of monitoring inevitably drops. Maine’s care facilities have faced criticism for lack of oversight, particularly when residents are at risk of wandering.
| Systemic Causes | Individual/Clinical Errors |
|---|---|
| Chronic Understaffing | Ignoring or silencing equipment alarms |
| Lack of Proper Training | Failing to interpret fetal heart strips correctly |
| Inadequate Facility Policies | Missing a scheduled vital sign check |
| “Profit over People” Business Models | Failing to advocate for a patient via the chain of command |
Communication and Handoff Errors
The “handoff”—when one shift ends and another begins—is the most dangerous time for a patient. If the outgoing nurse fails to mention that a patient was unusually confused or that their blood pressure was trending downward, the incoming nurse may not know to look for those specific warning signs.
Documentation is the backbone of monitoring. If it isn’t written down, in the eyes of the law, it didn’t happen. Furthermore, if a nurse notices a problem but the attending physician ignores it, the nurse has a duty to invoke the “chain of command.” Failing to escalate a concern to a supervisor is a common component of medical malpractice claims.
Proving Medical Malpractice for Monitoring Lapses
Proving that a failure to monitor occurred is a complex task. It requires more than just showing that something went wrong; it requires showing that the healthcare provider’s inaction (or delayed action) was a direct cause of the harm.
Legal Elements of a Claim
To win a case, we must establish four key elements:
- Duty: A provider-patient relationship existed (you were under their care).
- Breach: The provider failed to monitor according to the accepted standard of care.
- Causation: This failure directly caused the injury (for example, internal bleeding that would likely have been treatable if caught earlier).
- Damages: The patient suffered actual harm, such as additional medical bills, lost wages, or permanent disability.
Our team at Garmey Law carefully reviews nursing logs, monitor data, and results from similar cases to build a clear timeline of where the oversight happened. We often work with qualified medical experts who can explain what a reasonable provider should have noticed and how earlier intervention could have changed the outcome.
Compensation for Victims
Victims of monitoring negligence can seek compensation for both economic and non-economic damages. This can include:
- Medical Expenses: Past and future costs for treatment related to the injury.
- Lost Wages: Income lost while recovering or due to long-term disability.
- Pain and Suffering: The physical and emotional trauma caused by the neglect.
- Wrongful Death: If the failure to monitor resulted in the loss of a loved one.
While no amount of money can undo the damage, compensation can help families afford necessary care and can push institutions to prioritize patient safety.
Frequently Asked Questions about Patient Monitoring
How can I tell if I was inadequately monitored?
It can be hard to know for sure while you are in a hospital bed, but there are several “red flags” that suggest a failure to monitor:
- Did you feel “forgotten” or left alone for hours without a staff member checking your vitals?
- Did you or your family repeatedly press the call button for an urgent issue without a timely response?
- Did the staff seem overwhelmed, rushed, or distracted?
- Did a complication seem to come “out of nowhere” despite you complaining of symptoms for hours?
What are the most common injuries from monitoring failures?
When warning signs are missed, the body can deteriorate rapidly. Common injuries include:
- Brain Damage: Often from unmonitored oxygen levels or hypoglycemia.
- Sepsis and Organ Failure: From untreated infections.
- Stroke or Cardiac Arrest: When blood pressure or heart rhythm changes are ignored.
- Permanent Paralysis: Sometimes resulting from unmonitored post-op spinal complications.
What steps should I take if I suspect negligence?
If you suspect that you or a loved one suffered an injury or death because of a failure to monitor, take these steps:
- Prioritize Health: Ensure you and your loved ones are now in a safe environment receiving proper care.
- Gather Records: Request copies of your medical records, including nursing notes and vital sign flow sheets.
- Document Everything: Write down your memory of the timeline—when you felt symptoms, when you called for help, and who responded.
- Consult a Specialist: Contact a medical malpractice attorney like the attorneys at Garmey Law who understands the nuances of Maine law and healthcare standards.
Talk to Garmey Law About a Failure-to-Monitor Case
At Garmey Law, we believe every patient in Maine – from Portland to Brunswick and beyond – deserves the full attention of their medical team. Monitoring is not a luxury; it is a core requirement of safe medicine. When hospitals cut corners or staff fail to respond to warning signs, patients and families can suffer preventable harm.
If you or a loved one has suffered due to a healthcare provider’s failure to monitor, you deserve answers and accountability. Contact Garmey Law for a free, no-obligation consultation to discuss what happened and learn your legal options. More info about medical malpractice services